Tyrosinemia Type 1
Are you a genetic carrier for Tyrosinemia? Find out with this DNA Test.
- Detects four FAH variants linked to Tyrosinemia type I
- Characterized by elevated levels of the amino acid tyrosine
- Carrier screening test intended for couples who are planning to become pregnant
- 100% private and confidential online results
Already have DNA markers? Sign in and upload your data to view results.
Need to take the DNA Test? Order our easy-to-use swab kit.
Detailed Description
Tyrosinemia is an inherited metabolic disorder characterized by elevated levels of the amino acid tyrosine, a basic building block of most proteins. Based on symptoms and the underlying genetic cause tyrosinemia can be classified into three types.
Tyrosinemia Type 1 is most common in people of French Canadian, Finnish, Askenazi Jewish, Norwegian and Turkish descent. It is caused by genetic variation in the FAH gene, which gives instructions to make the fumarylacetoacetate hydrolase enzyme. This enzyme is involved in the last step of the pathway that breaks down tyrosine. Affected people with genetic variants produce an enzyme with reduced function leading to the build up of tyrosine and tyrosine byproducts inside cells.
Take this test to find out whether you are a genetic carrier for FAH variants and are at risk of passing it to your children. This is intended to be a carrier screening test for couples who are considering to start a family.
The Genetics
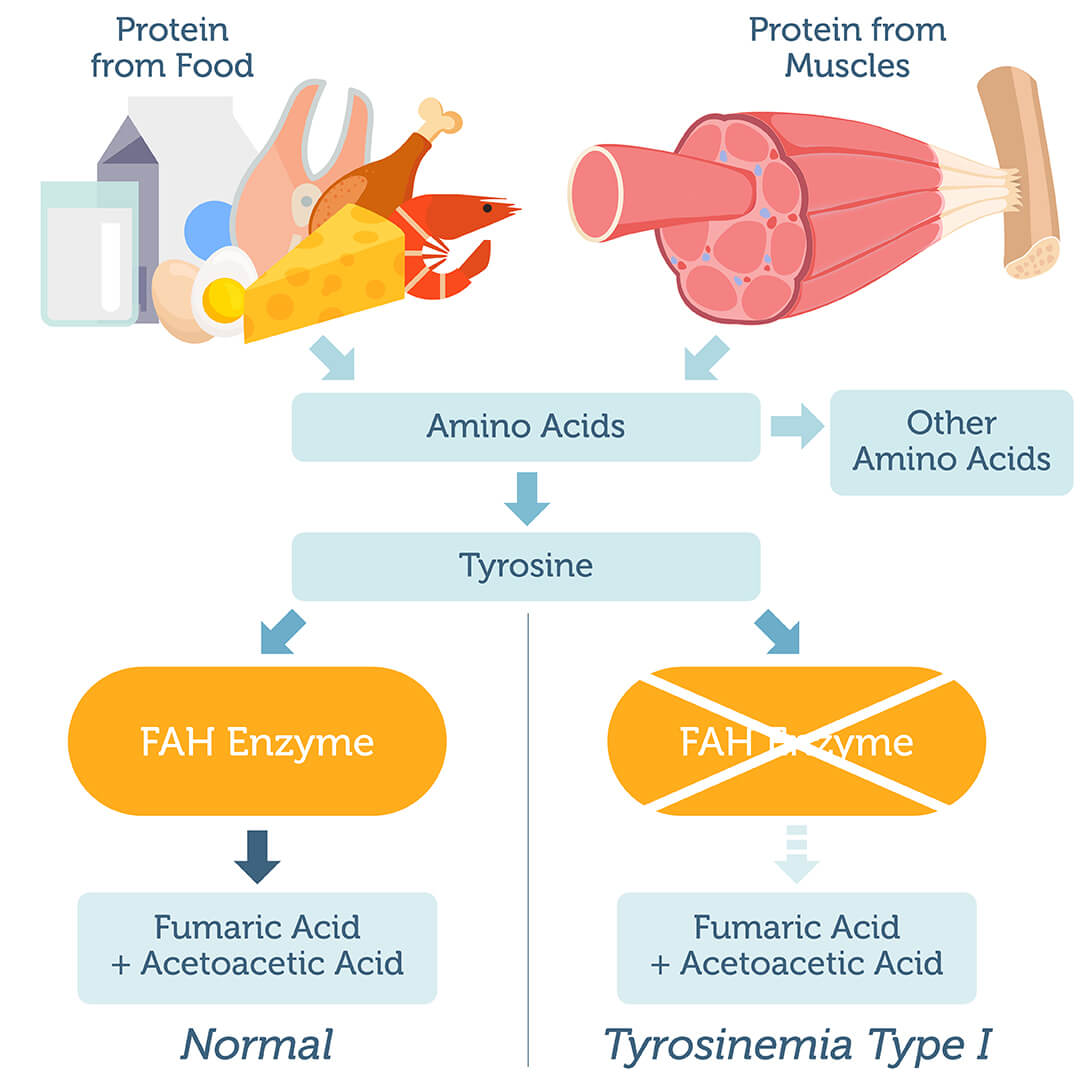
Tyrosinemia type I is caused by genetic variation in the FAH gene, which gives instructions to make the fumarylacetoacetate hydrolase enzyme. This enzyme is involved in the last step of the pathway that breaks down tyrosine. People with FAH variants produce non-functional protein, leading to build up of tyrosine and tyrosine byproducts in cells.
Tyrosinemia type I is inherited in an autosomal recessive pattern, which means two defective copies of the FAH gene must be inherited in order for symptoms to appear.

Variants Tested
This test looks at four genetic variants of the FAH gene that occur in >99% of Askenazi Jewish carriers, approximately 90% of French Canadian carriers and 86% of Finnish carriers of tyrosinemia type I.
- rs80338899
- rs80338898
- rs80338901
- rs80338895
Understanding your carrier status for these variants will help you understand the risk of passing it to your children.
While it provides a risk analysis for these conditions, it may be necessary to use gene and genome sequencing tests, as additional genetic variantsare linked to tyrosinemia.
Signs & Symptoms
- High level of tyrosine in blood
- Failure to thrive
- Liver problems (hepatomegaly, cirrhosis, liver failure)
- Kidney problems (tubular dysfunctions, glomerusclerosis)
- Neurologic crises (mental status change, abdominal pain, respiratory failure requiring mechanical ventilation)
- Higher liver cancer risk (especially in those who are diagnosed later, and don’t receive Nitisinone treatment as newborns)
- Impaired blood clotting (coagulation)
- Rickets
How It Works
Step 1: Sign up for a free Genebase account.
Step 2: Upload your DNA markers to Genebase.
Step 3: Login to your account to access your results when they are ready.